Search
- Page Path
- HOME > Search
- Thyroid
- Exploring the Association between Thyroid Function and Frailty: Insights from Representative Korean Data
- Youn-Ju Lee, Min-Hee Kim, Dong-Jun Lim, Jung-Min Lee, Sang Ah Chang, Jeongmin Lee
- Endocrinol Metab. 2023;38(6):729-738. Published online November 2, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1769
- 1,115 View
- 73 Download
- 1 Web of Science
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
This study investigates the association between thyroid function and frailty in the old patients using representative data.
Methods
The study was conducted using data from the Korea National Health and Nutrition Examination Survey conducted from 2013 to 2015. The study population included 2,416 participants aged 50 years and older with available thyroid function test data. Frailty assessment was performed using the Fried frailty phenotype. The prevalence of frailty was analyzed across different thyroid diseases and thyroid function parameters.
Results
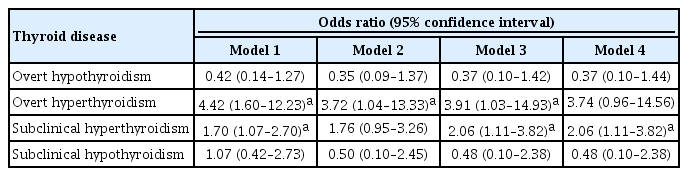
The significant association between thyroid dysfunction and frailty was observed in overt hyperthyroidism and subclinical hyperthyroidism. After adjusting for various factors, the association between thyroid dysfunction and frailty remained significant. On the other hand, overt hypothyroidism did not show a significant association with frailty in the adjusted analysis. For individuals with overt hyperthyroidism and subclinical hyperthyroidism, higher levels of free thyroxine (FT4) were significantly associated with an increased risk of frailty (aOR >999; 95% CI, >999 to 999). Among individuals with overt hypothyroidism, lower level of FT4 levels and high thyrotropin (TSH) levels showed a significant association with frailty risk (FT4: aOR, <0.01; TSH: aOR, 999). In participants with subclinical hypothyroidism, there were no significant associations between parameters for thyroid and frailty risk.
Conclusion
These findings suggest that thyroid dysfunction, particularly overt hyperthyroidism and subclinical hyperthyroidism, may be associated with an increased risk of frailty in the old patients. -
Citations
Citations to this article as recorded by- Associations of thyroid feedback quantile-based index with diabetes in euthyroid adults in the United States and China
Heng Wan, Genfeng Yu, Yajun He, Siyang Liu, Xingying Chen, Yuqi Jiang, Hualin Duan, Xu Lin, Lan Liu, Jie Shen
Annals of Medicine.2024;[Epub] CrossRef
- Associations of thyroid feedback quantile-based index with diabetes in euthyroid adults in the United States and China

- Thyroid
- Quality of Life of Survivors of Thyroid Cancer Is Not Inferior to That in Subjects without Cancer: Long-Term after Over 5 Years
- Jeongmin Lee, Youn-Ju Lee, Dong-Jun Lim, Jung-Min Lee, Sang-Ah Chang, Min-Hee Kim
- Endocrinol Metab. 2022;37(4):664-673. Published online August 29, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1499
- 3,176 View
- 184 Download
- 2 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
Patients with thyroid cancer undergo less extensive surgery and additional therapies compared to those with other cancers. We aimed to compare the quality of life (QoL) between patients with thyroid cancer and healthy subjects using representative data from Korea. Differences in QoL of thyroid cancer survivors according to the duration after cancer diagnosis was also evaluated.
Methods
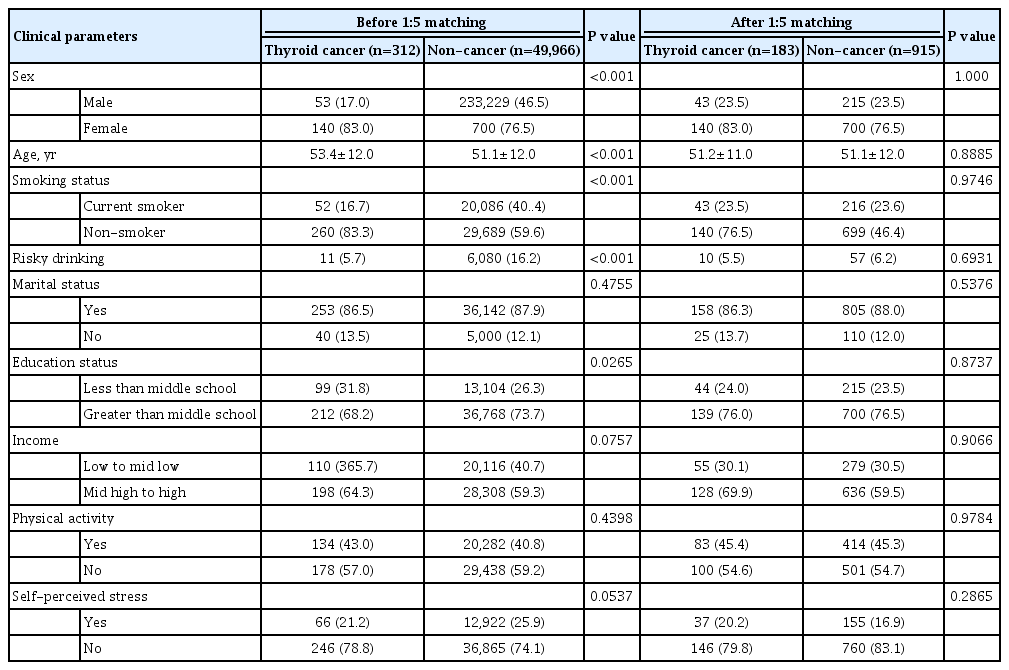
This population-based cohort study included 50,278 subjects who participated in the Korea National Health and Nutrition Examination Survey between 2007 and 2017. QoL was compared between patients with thyroid cancer and healthy subjects using self-reported data from the EuroQoL (EQ)-5 dimension (5D) and EQ-visual analog scale (VAS). Propensity score matching was used to match thyroid cancer survivors to healthy subjects (1:5 matching).
Results
Linear regression with univariate analysis showed that the presence of thyroid cancer was positively correlated with better EQ-5D index scores (β-coefficient=0.010, p=0.046). After adjusting for multiple covariables, statistical significance was maintained. EQ-VAS fails to demonstrate any significant correlation. Among the EQ-5D categories, patients with thyroid cancer showed better self-care than healthy subjects. Thyroid cancer duration did not correlate with the EQ-5D index score. In subgroup analyses, compared to patients with thyroid cancer duration of <5 years, no significant difference was observed in the correlation between the EQ-5D index score and survival duration in those with thyroid cancer duration of 5 to 9 years and ≥10 years.
Conclusion
Using a large-scale nationwide population-based database, our study demonstrated better QoL, especially in terms of self-care, among thyroid cancer survivors than among healthy subjects without cancer. -
Citations
Citations to this article as recorded by- Quality of Life Considerations in Patients Treated for Differentiated Thyroid Cancer
Jie Liu
Clinical Thyroidology.2023; 35(4): 160. CrossRef - The psychosocial impact of thyroid cancer
Parker Haymart, Nina Jackson Levin, Megan R. Haymart
Current Opinion in Endocrinology, Diabetes & Obesity.2023; 30(5): 252. CrossRef - Longitudinal Changes in Quality of Life Before and After Thyroidectomy in Patients With Differentiated Thyroid Cancer
Byung Hun Kim, Soo Rack Ryu, Jin Won Lee, Chang Myeon Song, Yong Bae Ji, Seok Hyun Cho, Seung Hwan Lee, Kyung Tae
The Journal of Clinical Endocrinology & Metabolism.2023;[Epub] CrossRef
- Quality of Life Considerations in Patients Treated for Differentiated Thyroid Cancer

- Miscellaneous
- Corrigendum: Correction of Acknowledgments. Protocol for a Korean Multicenter Prospective Cohort Study of Active Surveillance or Surgery (KoMPASS) in Papillary Thyroid Microcarcinoma
- Min Ji Jeon, Yea Eun Kang, Jae Hoon Moon, Dong Jun Lim, Chang Yoon Lee, Yong Sang Lee, Sun Wook Kim, Min-Hee Kim, Bo Hyun Kim, Ho-Cheol Kang, Minho Shong, Sun Wook Cho, Won Bae Kim
- Endocrinol Metab. 2022;37(1):181-182. Published online February 28, 2022
- DOI: https://doi.org/10.3803/EnM.2022.104
- Corrects: Endocrinol Metab 2021;36(2):359
- 2,810 View
- 110 Download
- 1 Web of Science
- 1 Crossref
-
 PDF
PDF PubReader
PubReader  ePub
ePub -
Citations
Citations to this article as recorded by- Risk of thyroid cancer associated with glucagon‐like peptide‐1 receptor agonists and dipeptidyl peptidase‐4 inhibitors in patients with type 2 diabetes: A population‐based cohort study
Sungho Bea, Heejun Son, Jae Hyun Bae, Sun Wook Cho, Ju‐Young Shin, Young Min Cho
Diabetes, Obesity and Metabolism.2024; 26(1): 108. CrossRef
- Risk of thyroid cancer associated with glucagon‐like peptide‐1 receptor agonists and dipeptidyl peptidase‐4 inhibitors in patients with type 2 diabetes: A population‐based cohort study

- Clinical Study
- Protocol for a Korean Multicenter Prospective Cohort Study of Active Surveillance or Surgery (KoMPASS) in Papillary Thyroid Microcarcinoma
- Min Ji Jeon, Yea Eun Kang, Jae Hoon Moon, Dong Jun Lim, Chang Yoon Lee, Yong Sang Lee, Sun Wook Kim, Min-Hee Kim, Bo Hyun Kim, Ho-Cheol Kang, Minho Shong, Sun Wook Cho, Won Bae Kim
- Endocrinol Metab. 2021;36(2):359-364. Published online March 23, 2021
- DOI: https://doi.org/10.3803/EnM.2020.890
- Correction in: Endocrinol Metab 2022;37(1):181

- 5,807 View
- 202 Download
- 17 Web of Science
- 17 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
A Korean Multicenter Prospective cohort study of Active Surveillance or Surgery (KoMPASS) for papillary thyroid microcarcinomas (PTMCs) has been initiated. The aim is to compare clinical outcomes between active surveillance (AS) and an immediate lobectomy for low-risk PTMCs. We here outline the detailed protocol for this study.
Methods
Adult patients with a cytopathologically confirmed PTMC sized 6.0 to 10.0 mm by ultrasound (US) will be included. Patients will be excluded if they have a suspicious extra-thyroidal extension or metastasis of a PTMC or multiple thyroid nodules or other thyroid diseases which require a total thyroidectomy. Printed material describing the prognosis of PTMCs, and the pros and cons of each management option, will be provided to eligible patients to select their preferred intervention. For the AS group, thyroid US, thyroid function, and quality of life (QoL) parameters will be monitored every 6 months during the first year, and then annually thereafter. Disease progression will be defined as a ≥3 mm increase in maximal diameter of a PTMC, or the development of new thyroid cancers or metastases. If progression is detected, patients should undergo appropriate surgery. For the lobectomy group, a lobectomy with prophylactic central neck dissection will be done within 6 months. After initial surgery, thyroid US, thyroid function, serum thyroglobulin (Tg), anti-Tg antibody, and QoL parameters will be monitored every 6 months during the first year and annually thereafter. Disease progression will be defined in these cases as the development of new thyroid cancers or metastases.
Conclusion
KoMPASS findings will help to confirm the role of AS, and develop individualized management strategies, for low-risk PTMCs. -
Citations
Citations to this article as recorded by- Active Surveillance for Low-Risk Thyroid Cancers: A Review of Current Practice Guidelines
Min Joo Kim, Jae Hoon Moon, Eun Kyung Lee, Young Shin Song, Kyong Yeun Jung, Ji Ye Lee, Ji-hoon Kim, Kyungsik Kim, Sue K. Park, Young Joo Park
Endocrinology and Metabolism.2024; 39(1): 47. CrossRef - It Is Time to Understand the Additional Benefits of Active Surveillance for Low-Risk Papillary Thyroid Carcinoma
Kyeong Jin Kim
Endocrinology and Metabolism.2024; 39(1): 95. CrossRef - Active Surveillance for Low-Risk Papillary Thyroid Carcinoma as an Acceptable Management Option with Additional Benefits: A Comprehensive Systematic Review
Jee Hee Yoon, Wonsuk Choi, Ji Yong Park, A Ram Hong, Hee Kyung Kim, Ho-Cheol Kang
Endocrinology and Metabolism.2024; 39(1): 152. CrossRef - Active Surveillance for Low-Risk Papillary Thyroid Carcinoma as an Acceptable Management Option with Additional Benefits: A Comprehensive Systematic Review
Jee Hee Yoon, Wonsuk Choi, Ji Yong Park, A Ram Hong, Hee Kyung Kim, Ho-Cheol Kang
Endocrinology and Metabolism.2024; 39(1): 152. CrossRef - Thyroid‐Stimulating Hormone, Age, and Tumor Size are Risk Factors for Progression During Active Surveillance of Low‐Risk Papillary Thyroid Microcarcinoma in Adults
Yasuhiro Ito, Akira Miyauchi, Makoto Fujishima, Takuya Noda, Tsutomu Sano, Takahiro Sasaki, Taketoshi Kishi, Tomohiko Nakamura
World Journal of Surgery.2023; 47(2): 392. CrossRef - Thyroid FNA cytology: The Eastern versus Western perspectives
Mitsuyoshi Hirokawa, Manon Auger, Chan Kwon Jung, Fabiano Mesquita Callegari
Cancer Cytopathology.2023; 131(7): 415. CrossRef - To Screen or Not to Screen?
Do Joon Park
Endocrinology and Metabolism.2023; 38(1): 69. CrossRef - Lower Thyroid Cancer Mortality in Patients Detected by Screening: A Meta-Analysis
Shinje Moon, Young Shin Song, Kyong Yeun Jung, Eun Kyung Lee, Young Joo Park
Endocrinology and Metabolism.2023; 38(1): 93. CrossRef - Long-Term Outcomes of Active Surveillance and Immediate Surgery for Adult Patients with Low-Risk Papillary Thyroid Microcarcinoma: 30-Year Experience
Akira Miyauchi, Yasuhiro Ito, Makoto Fujishima, Akihiro Miya, Naoyoshi Onoda, Minoru Kihara, Takuya Higashiyama, Hiroo Masuoka, Shiori Kawano, Takahiro Sasaki, Mitsushige Nishikawa, Shuji Fukata, Takashi Akamizu, Mitsuru Ito, Eijun Nishihara, Mako Hisakad
Thyroid®.2023; 33(7): 817. CrossRef - Active Surveillance Outcomes of Patients with Low-Risk Papillary Thyroid Microcarcinoma According to Levothyroxine Treatment Status
Masashi Yamamoto, Akira Miyauchi, Yasuhiro Ito, Makoto Fujishima, Takahiro Sasaki, Takumi Kudo
Thyroid®.2023; 33(10): 1182. CrossRef - Cost-Effectiveness of Active Surveillance Compared to Early Surgery of Small Papillary Thyroid Cancer: A Retrospective Study on a Korean Population
Han-Sang Baek, Jeonghoon Ha, Kwangsoon Kim, Jaseong Bae, Jeong Soo Kim, Sungju Kim, Dong-Jun Lim, Chulmin Kim
Journal of Korean Medical Science.2023;[Epub] CrossRef - Optimal Cutoff Values of the Contact Angle of Tumor on Sonography System for Predicting Extrathyroidal Extension of Papillary Thyroid Carcinoma by Tumor Location
Ik Beom Shin, Do Hoon Koo, Dong Sik Bae
Clinical Medicine Insights: Oncology.2023;[Epub] CrossRef - Thermal ablation for papillary thyroid microcarcinoma located in the isthmus: a study with 3 years of follow-up
Lin Zheng, Fang-yi Liu, Jie Yu, Zhi-gang Cheng, Xiao-ling Yu, Xiao-cong Dong, Zhi-yu Han, Ping Liang
Future Oncology.2022; 18(4): 471. CrossRef - Trends in the Management of Localized Papillary Thyroid Carcinoma in the United States (2000–2018)
Elisa Pasqual, Julie Ann Sosa, Yingxi Chen, Sara J. Schonfeld, Amy Berrington de González, Cari M. Kitahara
Thyroid.2022; 32(4): 397. CrossRef - Management of Low-Risk Thyroid Cancers: Is Active Surveillance a Valid Option? A Systematic Review of the Literature
Renato Patrone, Nunzio Velotti, Stefania Masone, Alessandra Conzo, Luigi Flagiello, Chiara Cacciatore, Marco Filardo, Vincenza Granata, Francesco Izzo, Domenico Testa, Stefano Avenia, Alessandro Sanguinetti, Andrea Polistena, Giovanni Conzo
Journal of Clinical Medicine.2021; 10(16): 3569. CrossRef - Cost-Effectiveness Analysis of Active Surveillance Compared to Early Surgery in Small Papillary Thyroid Cancer: A Systemic Review
Han-sang Baek, Chai-ho Jeong, Jeonghoon Ha, Ja-Seong Bae, Jeong-soo Kim, Dong-Jun Lim, Chul-Min Kim
Cancer Management and Research.2021; Volume 13: 6721. CrossRef - Active Surveillance as an Effective Management Option for Low-Risk Papillary Thyroid Microcarcinoma
Min Ji Jeon, Won Gu Kim, Tae Yong Kim, Young Kee Shong, Won Bae Kim
Endocrinology and Metabolism.2021; 36(4): 717. CrossRef
- Active Surveillance for Low-Risk Thyroid Cancers: A Review of Current Practice Guidelines

- Clinical Study
- Comparison of Natural Course between Thyroid Cancer Nodules and Thyroid Benign Nodules
- Kyun-Jin Yun, Jeonghoon Ha, Min-Hee Kim, Ye Young Seo, Mee Kyoung Kim, Hyuk-Sang Kwon, Ki-Ho Song, Moo Il Kang, Ki-Hyun Baek
- Endocrinol Metab. 2019;34(2):195-202. Published online June 24, 2019
- DOI: https://doi.org/10.3803/EnM.2019.34.2.195
- 4,513 View
- 65 Download
- 8 Web of Science
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub Background The natural course of thyroid cancer nodules and benign nodules is different. This study was to compare the changes in size between thyroid cancer nodules and thyroid benign nodules. The risk factors associated with the changes of thyroid cancer nodules were assessed.
Methods This study contains retrospective observational and prospective analysis. A total of 113 patients with 120 nodules were recruited in the cancer group, and 116 patients with 119 nodules were enrolled in the benign group. Thyroid ultrasonography was performed at least two times at more than 1-year interval.
Results The mean follow-up durations were 29.5±18.8 months (cancer group) and 31.9±15.8 months (benign group) (
P =0.32). The maximum diameter change in length was 0.36±0.97 mm/year in the cancer group and –0.04±0.77 mm/year in the benign group (P <0.01). The volume was significantly increased in the cancer group compared with the benign group (0.06±0.18 mL/year vs. 0.004±0.05 mL/year, respectively,P <0.01; 26.9%±57.9%/year vs. 1.7%±26.0%/year,P <0.01). Initial maximum diameter (β=0.02,P <0.01) and initial volume (β=0.13,P <0.01) were significantly associated with volume change (mL)/year. Initial maximum standardized uptake value did not predict the nodule growth.Conclusion It is suggested that thyroid cancer nodules progress rapidly compared with benign nodules. Initial size and volume of nodule were independent risk factors for cancer nodule growth.
-
Citations
Citations to this article as recorded by- RAS-Mutated Cytologically Indeterminate Thyroid Nodules: Prevalence of Malignancy and Behavior Under Active Surveillance
Hannah J. Sfreddo, Elizabeth S. Koh, Karena Zhao, Christina E. Swartzwelder, Brian R. Untch, Jennifer L. Marti, Benjamin R. Roman, Jared Dublin, Ronald S. Wang, Rong Xia, Jean-Marc Cohen, Bin Xu, Ronald Ghossein, Babak Givi, Jay O. Boyle, R. Michael Tuttl
Thyroid®.2024;[Epub] CrossRef - Ultrasound for the assessment of thyroid nodules: an overview for non-radiologists
Conor Hamill, Peter Ellis, Philip C Johnston
British Journal of Hospital Medicine.2022; 83(7): 1. CrossRef - Цитологічно підтверджений вузловий зоб у членів Українсько-Американського когортного дослідження: дескриптивний аналіз результатів обстеження за 1998- 2015 роки
M.D. Tronko, L.S. Strafun, H.M. Terekhova, H.A. Zamotayeva, I.P. Pasteur
Endokrynologia.2022; 27(1): 5. CrossRef - A Computational Study on the Role of Parameters for Identification of Thyroid Nodules by Infrared Images (and Comparison with Real Data)
José R. González, Charbel Damião, Maira Moran, Cristina A. Pantaleão, Rubens A. Cruz, Giovanna A. Balarini, Aura Conci
Sensors.2021; 21(13): 4459. CrossRef - Ultrasound in active surveillance for low-risk papillary thyroid cancer: imaging considerations in case selection and disease surveillance
Sangeet Ghai, Ciara O’Brien, David P. Goldstein, Anna M. Sawka, Lorne Rotstein, Dale Brown, John de Almeida, Patrick Gullane, Ralph Gilbert, Douglas Chepeha, Jonathan Irish, Jesse Pasternak, Shereen Ezzat, James P. Brierley, Richard W. Tsang, Eric Monteir
Insights into Imaging.2021;[Epub] CrossRef - Association between various thyroid gland diseases, TSH values and thyroid cancer: a case–control study
Leif Schiffmann, Karel Kostev, Matthias Kalder
Journal of Cancer Research and Clinical Oncology.2020; 146(11): 2989. CrossRef - Combination of peroxisome proliferator–activated receptor gamma and retinoid X receptor agonists induces sodium/iodide symporter expression and inhibits cell growth of human thyroid cancer cells
Jui-Yu Chen, Jane-Jen Wang, Hsin-Chen Lee, Chin-Wen Chi, Chen-Hsen Lee, Yi-Chiung Hsu
Journal of the Chinese Medical Association.2020; 83(10): 923. CrossRef - Growth rates of malignant and benign thyroid nodules in an ultrasound follow-up study: a retrospective cohort study
Michael Cordes, Theresa Ida Götz, Karen Horstrup, Torsten Kuwert, Christian Schmidkonz
BMC Cancer.2019;[Epub] CrossRef
- RAS-Mutated Cytologically Indeterminate Thyroid Nodules: Prevalence of Malignancy and Behavior Under Active Surveillance

- Clinical Study
- Obesity and Hyperglycemia in Korean Men with Klinefelter Syndrome: The Korean Endocrine Society Registry
- Seung Jin Han, Kyung-Soo Kim, Wonjin Kim, Jung Hee Kim, Yong-ho Lee, Ji Sun Nam, Ji A Seo, Bu Kyung Kim, Jihyun Lee, Jin Ook Chung, Min-Hee Kim, Tae-Seo Sohn, Han Seok Choi, Seong Bin Hong, Yoon-Sok Chung
- Endocrinol Metab. 2016;31(4):598-603. Published online December 20, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.4.598
- 5,295 View
- 35 Download
- 20 Web of Science
- 18 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background The aim of this study was to investigate the prevalence of obesity in Korean men with Klinefelter syndrome (KS) and the associated risk factors for obesity and hyperglycemia.
Methods Data were collected retrospectively from medical records from 11 university hospitals in Korea between 1994 and 2014. Subjects aged ≥18 years with newly diagnosed KS were enrolled. The following parameters were recorded at baseline before treatment: chief complaint, height, weight, fasting glucose level, lipid panel, blood pressure, testosterone, luteinizing hormone, follicle-stimulating hormone, karyotyping patterns, and history of hypertension, diabetes, and dyslipidemia.
Results Data were analyzed from 376 of 544 initially enrolled patients. The rate of the 47 XXY chromosomal pattern was 94.1%. The prevalence of obesity (body mass index ≥25 kg/m2) in Korean men with KS was 42.6%. The testosterone level was an independent risk factor for obesity and hyperglycemia.
Conclusion Obesity is common in Korean men with KS. Hypogonadism in patients with KS was associated with obesity and hyperglycemia.
-
Citations
Citations to this article as recorded by- A dual-center study of predictive factors for sperm retrieval through microdissection testicular sperm extraction and intracytoplasmic sperm injection outcomes in men with non-mosaic Klinefelter syndrome
Jong Hyeun Baeck, Tae Jin Kim, Tae Heon Kim, Seung-Ryeol Lee, Dong Soo Park, Hwang Kwon, Ji Eun Shin, Dong Hyeon Lee, Young Dong Yu
Investigative and Clinical Urology.2023; 64(1): 41. CrossRef - Cardiorespiratory fitness in adolescents and young adults with Klinefelter syndrome – a pilot study
Julia Spiekermann, Kathrin Sinningen, Beatrice Hanusch, Michaela Kleber, Michael M. Schündeln, Cordula Kiewert, Heide Siggelkow, Jakob Höppner, Corinna Grasemann
Frontiers in Endocrinology.2023;[Epub] CrossRef - Metabolic Profile in a Cohort of Young Sicilian Patients with Klinefelter’s Syndrome: The Role of Irisin
Stefano Radellini, Valentina Guarnotta, Vincenzo Sciabica, Giuseppe Pizzolanti, Carla Giordano, Vito Angelo Giagulli
International Journal of Endocrinology.2022; 2022: 1. CrossRef - Metabolic and Nutritional Aspects in Paediatric Patients with Klinefelter Syndrome: A Narrative Review
Chiara Mameli, Giulia Fiore, Arianna Sangiorgio, Marta Agostinelli, Giulia Zichichi, Gianvincenzo Zuccotti, Elvira Verduci
Nutrients.2022; 14(10): 2107. CrossRef - Klinefelter syndrome in an adolescent with severe obesity, insulin resistance, and hyperlipidemia, successfully treated with testosterone replacement therapy
Shota Fukuhara, Jun Mori, Hisakazu Nakajima
Clinical Pediatric Endocrinology.2021; 30(3): 127. CrossRef - Glucose metabolic disorder in Klinefelter syndrome: a retrospective analysis in a single Chinese hospital and literature review
Shixuan Liu, Tao Yuan, Shuoning Song, Shi Chen, Linjie Wang, Yong Fu, Yingyue Dong, Yan Tang, Weigang Zhao
BMC Endocrine Disorders.2021;[Epub] CrossRef - What Every Internist-Endocrinologist Should Know about Rare Genetic Syndromes in Order to Prevent Needless Diagnostics, Missed Diagnoses and Medical Complications: Five Years of ‘Internal Medicine for Rare Genetic Syndromes’
Anna G. W. Rosenberg, Minke R. A. Pater, Karlijn Pellikaan, Kirsten Davidse, Anja A. Kattentidt-Mouravieva, Rogier Kersseboom, Anja G. Bos-Roubos, Agnies van Eeghen, José M. C. Veen, Jiske J. van der Meulen, Nina van Aalst-van Wieringen, Franciska M. E. H
Journal of Clinical Medicine.2021; 10(22): 5457. CrossRef - Klinefelter Syndrome and Diabetes
Mark J. O’Connor, Emma A. Snyder, Frances J. Hayes
Current Diabetes Reports.2019;[Epub] CrossRef - Endocrine aspects of Klinefelter syndrome
Adriana Herrera Lizarazo, Michelle McLoughlin, Maria G. Vogiatzi
Current Opinion in Endocrinology, Diabetes & Obesity.2019; 26(1): 60. CrossRef - Sex differences in metabolism and cardiometabolic disorders
Karthickeyan Chella Krishnan, Margarete Mehrabian, Aldons J. Lusis
Current Opinion in Lipidology.2018; 29(5): 404. CrossRef - Klinefelter Syndrome: Integrating Genetics, Neuropsychology, and Endocrinology
Claus H Gravholt, Simon Chang, Mikkel Wallentin, Jens Fedder, Philip Moore, Anne Skakkebæk
Endocrine Reviews.2018; 39(4): 389. CrossRef - Sex differences in obesity, lipid metabolism, and inflammation—A role for the sex chromosomes?
Temeka Zore, Maria Palafox, Karen Reue
Molecular Metabolism.2018; 15: 35. CrossRef - Klinefelter syndrome, insulin resistance, metabolic syndrome, and diabetes: review of literature and clinical perspectives
Andrea Salzano, Roberta D’Assante, Liam M. Heaney, Federica Monaco, Giuseppe Rengo, Pietro Valente, Daniela Pasquali, Eduardo Bossone, Daniele Gianfrilli, Andrea Lenzi, Antonio Cittadini, Alberto M. Marra, Raffaele Napoli
Endocrine.2018; 61(2): 194. CrossRef - Síndrome de Klinefelter y riesgo cardiovascular
A. Yamaguchi, P. Knoblovits
Hipertensión y Riesgo Vascular.2018; 35(4): 195. CrossRef - Articles inEndocrinology and Metabolismin 2016
Won-Young Lee
Endocrinology and Metabolism.2017; 32(1): 62. CrossRef - Sex differences in obesity: X chromosome dosage as a risk factor for increased food intake, adiposity and co-morbidities
Karen Reue
Physiology & Behavior.2017; 176: 174. CrossRef - Klinefelter Syndrome with Morbid Obesity Before Bariatric Surgery: A Case Report
Parisa Janmohammadi, Gholamreza Mohammadi-Farsani, Hana Arghavani, Mahmoud Arshad, Tayebeh Mokhber
Journal of Minimally Invasive Surgical Sciences.2017;[Epub] CrossRef - Klinefelter Syndrome and Metabolic Disorder
Ji Cheol Bae
Endocrinology and Metabolism.2016; 31(4): 535. CrossRef
- A dual-center study of predictive factors for sperm retrieval through microdissection testicular sperm extraction and intracytoplasmic sperm injection outcomes in men with non-mosaic Klinefelter syndrome

- Thyroid
- Cholestyramine Use for Rapid Reversion to Euthyroid States in Patients with Thyrotoxicosis
- Jeonghoon Ha, Kwanhoon Jo, Borami Kang, Min-Hee Kim, Dong-Jun Lim
- Endocrinol Metab. 2016;31(3):476-479. Published online July 26, 2016
- DOI: https://doi.org/10.3803/EnM.2016.31.3.476
- 3,893 View
- 51 Download
- 6 Web of Science
- 7 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Cholestyramine (CS) is an ion exchange resin, which binds to iodothyronines and would lower serum thyroid hormone level. The use of CS added to conventional antithyroid drugs to control thyrotoxicosis has been applied since 1980's, and several studies indicate that using CS in combination with methimazole (MZ) produces a more rapid decline in serum thyroid hormones than with only MZ treatment. Our recent retrospective review of five patients taking high dose MZ and CS, compared to age-, gender-, initial free thyroxine (T4) level-, and MZ dose-matched 12 patients with MZ use only, showed more rapid decline of both free T4 and triiodothyronine levels without more adverse events. CS could be safely applicable short-term adjunctive therapy when first-line antithyroid medications are not enough to adequately control severe thyrotoxicosis or side effects of antithyroid drug would be of great concern.
-
Citations
Citations to this article as recorded by- Therapeutic plasma exchange for Graves’ disease in pregnancy
Matthew Lumchee, Mimi Yue, Josephine Laurie, Adam Morton
Obstetric Medicine.2023; 16(2): 126. CrossRef - Ventricular arrhythmias, antiarrhythmic therapy and thyroidal illness in advanced heart failure: a case report and review of the literature
Fatima Alsalama, Salma Alzaabi, Cynthia Salloum, Marilyne Abi Younes, Feras Bader, Hussam Ghalib, Bassam Atallah
Drugs & Therapy Perspectives.2023; 39(4): 147. CrossRef - Amiodarone Induced Thyrotoxicosis and Treatment Complications in a Man With Cyanotic Congenital Heart Disease: A Case Report
Marvin Wei Jie Chua, Shao Feng Mok
Frontiers in Cardiovascular Medicine.2020;[Epub] CrossRef - Propylthiouracil-induced agranulocytosis as a rare complication of antithyroid drugs in a patient with Graves’ disease
Patrícia Novais Rabelo, Paula Novais Rabelo, Allyne Fernanda de Paula, Samuel Amanso da Conceição, Daniela Pultrini Pereira de Oliveira Viggiano, Daniela Espíndola Antunes, Estela Muszkat Jatene, Sílvia Leda França Moura de Paula, Monike Lourenço Dias, Ma
Revista da Associação Médica Brasileira.2019; 65(6): 755. CrossRef - Notes on Trauma-Related Thyroid Storm in the Emergency Department
Adam Morton
The Journal of Emergency Medicine.2018; 54(2): e35. CrossRef - Risk of embryopathies with use of antithyroidal medications
Stine L. Andersen
Current Opinion in Endocrinology, Diabetes & Obesity.2017; 24(5): 364. CrossRef - Thiamazole
Reactions Weekly.2017; 1644(1): 291. CrossRef
- Therapeutic plasma exchange for Graves’ disease in pregnancy

- Thyroid
- Refractory Graves' Disease Successfully Cured by Adjunctive Cholestyramine and Subsequent Total Thyroidectomy
- Yeoree Yang, Seawon Hwang, Minji Kim, Yejee Lim, Min-Hee Kim, Sohee Lee, Dong-Jun Lim, Moo-Il Kang, Bong-Yun Cha
- Endocrinol Metab. 2015;30(4):620-625. Published online December 31, 2015
- DOI: https://doi.org/10.3803/EnM.2015.30.4.620
- 4,409 View
- 85 Download
- 15 Web of Science
- 13 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader The three major forms of treatment for Graves thyrotoxicosis are antithyroid drugs, radioactive iodine therapy and thyroidectomy. Surgery is the definitive treatment for Graves thyrotoxicosis that is generally recommended when other treatments have failed or are contraindicated. Generally, thyrotoxic patients should be euthyroid before surgery to minimize potential complications which usually requires preoperative management with thionamides or inorganic iodine. But several cases of refractory Graves' disease have shown resistance to conventional treatment. Here we report a 40-year-old female patient with Graves' disease who complained of thyrotoxic symptoms for 7 months. Her thyroid function test and thyroid autoantibody profiles were consistent with Graves' disease. One kind of thionamides and β-blocker were started to control her disease. However, she was resistant to nearly all conventional medical therapies, including β-blockers, inorganic iodine, and two thionamides. She experienced hepatotoxicity from the thionamides. What was worse is her past history of serious allergic reaction to corticosteroids, which are often used to help control symptoms. A 2-week regimen of high-dose cholestyramine improved her uncontrolled thyrotoxicosis and subsequent thyroidectomy was successfully performed. In conclusion, cholestyramine could be administered as an effective and safe adjunctive agent for preoperative preparation in patients with severe hyperthyroid Graves's disease that is resistant to conventional therapies.
-
Citations
Citations to this article as recorded by- Enhanced predictive validity of integrative models for refractory hyperthyroidism considering baseline and early therapy characteristics: a prospective cohort study
Xinpan Wang, Tiantian Li, Yue Li, Qiuyi Wang, Yun Cai, Zhixiao Wang, Yun Shi, Tao Yang, Xuqin Zheng
Journal of Translational Medicine.2024;[Epub] CrossRef - Non-thionamide antithyroid drug options in Graves’ hyperthyroidism
Aliya Ruslan, Onyebuchi E Okosieme
Expert Review of Endocrinology & Metabolism.2023; 18(1): 67. CrossRef - Gestione clinica dell’ipertiroidismo refrattario
Daniela Gallo, Federica Martina Bianchi, Francesca Manzella La Barbera, Ilaria Clementi, Adriana Lai, Eliana Piantanida, Maria Laura Tanda
L'Endocrinologo.2023; 24(2): 167. CrossRef - Carbimazole-Resistant Grave’s Thyrotoxicosis is a Diagnostic and Therapeutic Dilemma, Case Report with Literature Review
Fateen Ata, Adeel Ahmad Khan, Shuja Tahir, Zaina Al Amer
International Medical Case Reports Journal.2023; Volume 16: 783. CrossRef - Medical treatment of thyrotoxicosis
Lorenzo SCAPPATICCIO, Giuseppe BELLASTELLA, Maria I. MAIORINO, Luca GIOVANELLA, Katherine ESPOSITO
The Quarterly Journal of Nuclear Medicine and Molecular Imaging.2021;[Epub] CrossRef - THERAPEUTIC EFFECTS OF COMBINATION REGIMENS INCLUDING METHIMAZOLE ON GRAVES HYPERTHYROIDISM: A NETWORK META-ANALYSIS OF RANDOMIZED CONTROLLED TRIALS
Maorong Wang, Yerong Yu
Endocrine Practice.2020; 26(6): 675. CrossRef - Cholestyramine alters bile acid amounts and the expression of cholesterol‐related genes in rabbit intestinal and hepatic tissues
Dong Ni Qiu, Quan Shang, Da Yu Sun, Wei Qun Ding, Zhong Guang Luo, Jian Chen, Wei Ru Jiang, Jian Ping Huang, Xiao Yun Jiang
Journal of Digestive Diseases.2017; 18(2): 107. CrossRef - ENDOCRINOLOGY IN PREGNANCY: Pregnancy and the incidence, diagnosing and therapy of Graves’ disease
Peter Laurberg, Stine Linding Andersen
European Journal of Endocrinology.2016; 175(5): R219. CrossRef - 2016 American Thyroid Association Guidelines for Diagnosis and Management of Hyperthyroidism and Other Causes of Thyrotoxicosis
Douglas S. Ross, Henry B. Burch, David S. Cooper, M. Carol Greenlee, Peter Laurberg, Ana Luiza Maia, Scott A. Rivkees, Mary Samuels, Julie Ann Sosa, Marius N. Stan, Martin A. Walter
Thyroid.2016; 26(10): 1343. CrossRef - Cholestyramine Use for Rapid Reversion to Euthyroid States in Patients with Thyrotoxicosis
Jeonghoon Ha, Kwanhoon Jo, Borami Kang, Min-Hee Kim, Dong-Jun Lim
Endocrinology and Metabolism.2016; 31(3): 476. CrossRef - The role of bile acids in metabolic regulation
Libor Vítek, Martin Haluzík
Journal of Endocrinology.2016; 228(3): R85. CrossRef - Recent Advances in Autoimmune Thyroid Diseases
Won Sang Yoo, Hyun Kyung Chung
Endocrinology and Metabolism.2016; 31(3): 379. CrossRef - A Case of Methimazole-Resistant Severe Graves' Disease: Dramatic Response to Cholestyramine
Seung Byung Chae, Eun Sook Kim, Yun Im Lee, Bo Ram Min
International Journal of Thyroidology.2016; 9(2): 190. CrossRef
- Enhanced predictive validity of integrative models for refractory hyperthyroidism considering baseline and early therapy characteristics: a prospective cohort study

- Thyroid
- Accelerated Disease Progression after Discontinuation of Sorafenib in a Patient with Metastatic Papillary Thyroid Cancer
- Kyung-Jin Yun, Woohyeon Kim, Eun Hee Kim, Min-Hee Kim, Dong-Jun Lim, Moo-Il Kang, Bong-Yun Cha
- Endocrinol Metab. 2014;29(3):388-393. Published online September 25, 2014
- DOI: https://doi.org/10.3803/EnM.2014.29.3.388
- 3,562 View
- 30 Download
- 23 Web of Science
- 22 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Distant metastases from papillary thyroid carcinoma (PTC) are rare and are associated with a poor prognosis. Here, we describe a patient with metastatic PTC who was treated with a tyrosine kinase inhibitor (TKI, sorafenib) for several months that was acutely exacerbated by discontinuation. A 43-year-old male was diagnosed with PTC in February 2004 and underwent total thyroidectomy followed by two courses of high-dose radioactive iodine (RAI) therapy. Despite two additional courses of high-dose RAI therapy, lung and muscle metastases were developed. Treatment with sorafenib was begun in September 2010. After 11 months treatment of sorafenib, newly developed metastatic lesions were found in mediastinal lymph nodes, liver, and bones. Considered as treatment failure, the administration of sorafenib was discontinued. Two weeks after sorafenib treatment was stopped, the disease progressed abruptly and caused death of the patient by respiratory failure. In our patient, PTC progressed rapidly after the cessation of sorafenib treatment. Patients with several other types of cancer have also experienced such rapid disease progression, termed "flare-ups." Physicians should be aware that flare-ups may occur in advanced PTC patients following the cessation of TKI therapy.
-
Citations
Citations to this article as recorded by- Lenvatinib: an investigational agent for the treatment of differentiated thyroid cancer
Silvia Martina Ferrari, Giusy Elia, Francesca Ragusa, Sabrina Rosaria Paparo, Valeria Mazzi, Mario Miccoli, Maria Rosaria Galdiero, Gilda Varricchi, Rudy Foddis, Giovanni Guglielmi, Claudio Spinelli, Concettina La Motta, Salvatore Benvenga, Alessandro Ant
Expert Opinion on Investigational Drugs.2021; 30(9): 913. CrossRef - Low Dose of Lenvatinib Treatment for Patients of Radioiodine-Refractory Differentiated Thyroid Carcinoma – A Real-World Experience
He-Jiun Jiang, Yen-Hsiang Chang, Yen-Hao Chen, Che-Wei Wu, Pei-Wen Wang, Pi-Jung Hsiao
Cancer Management and Research.2021; Volume 13: 7139. CrossRef - Rapid disease progression after discontinuation of lenvatinib in thyroid cancer
Haruhiko Yamazaki, Kiminori Sugino, Kenichi Matsuzu, Chie Masaki, Junko Akaishi, Kiyomi Hames, Chisato Tomoda, Akifumi Suzuki, Takashi Uruno, Keiko Ohkuwa, Wataru Kitagawa, Mitsuji Nagahama, Munetaka Masuda, Koichi Ito
Medicine.2020; 99(11): e19408. CrossRef - Lenvatinib for thyroid cancer treatment: discovery, pre-clinical development and clinical application
Rosa Maria Paragliola, Andrea Corsello, Valeria Del Gatto, Giampaolo Papi, Alfredo Pontecorvi, Salvatore Maria Corsello
Expert Opinion on Drug Discovery.2020; 15(1): 11. CrossRef - Efficacy and Limitations of Lenvatinib Therapy for Radioiodine-Refractory Differentiated Thyroid Cancer: Real-World Experiences
Chie Masaki, Kiminori Sugino, Naoko Saito, Junko Akaishi, Kiyomi Y. Hames, Chisato Tomoda, Akifumi Suzuki, Kenichi Matsuzu, Takashi Uruno, Keiko Ohkuwa, Wataru Kitagawa, Mitsuji Nagahama, Koichi Ito
Thyroid.2020; 30(2): 214. CrossRef - Papillary thyroid carcinoma with hyperthyroidism and multiple metastases
Li-li Zhang, Bin Liu, Fang-fang Sun, Hong-yu Li, Shuang Li, Li-rong Zhao
Medicine.2020; 99(30): e21346. CrossRef - Missing Skeletal Muscle Metastases of Papillary Thyroid Carcinoma
Leszek Herbowski
Diagnostics.2020; 10(7): 457. CrossRef - Reply to “Missing Skeletal Muscle Metastases of Papillary Thyroid Carcinoma”
Liviu Hitu, Calin Cainap, Dragos Apostu, Katalin Gabora, Eduard-Alexandru Bonci, Marius Badan, Alexandru Mester, Andra Piciu
Diagnostics.2020; 10(7): 458. CrossRef - Hif-1α Inhibitors Could Successfully Inhibit the Progression of Differentiated Thyroid Cancer in Vitro
Min-Hee Kim, Tae Hyeong Lee, Jin Soo Lee, Dong-Jun Lim, Peter Chang-Whan Lee
Pharmaceuticals.2020; 13(9): 208. CrossRef - Extended Real-World Observation of Patients Treated with Sorafenib for Radioactive Iodine-Refractory Differentiated Thyroid Carcinoma and Impact of Lenvatinib Salvage Treatment: A Korean Multicenter Study
Hye-Seon Oh, Dong Yeob Shin, Mijin Kim, So Young Park, Tae Hyuk Kim, Bo Hyun Kim, Eui Young Kim, Won Bae Kim, Jae Hoon Chung, Young Kee Shong, Dong Jun Lim, Won Gu Kim
Thyroid.2019; 29(12): 1804. CrossRef - Rapid pleural effusion after discontinuation of lenvatinib in a patient with pleural metastasis from thyroid cancer
Taisuke Uchida, Hideki Yamaguchi, Kazuhiro Nagamine, Tadato Yonekawa, Eriko Nakamura, Nobuhiro Shibata, Fumiaki Kawano, Yujiro Asada, Masamitsu Nakazato
Endocrinology, Diabetes & Metabolism Case Reports.2019;[Epub] CrossRef - Thyroid Disorders in the Elderly
Kevin Higgins
Clinics in Geriatric Medicine.2018; 34(2): 259. CrossRef - Treatment of refractory thyroid cancer
Amandine Berdelou, Livia Lamartina, Michele Klain, Sophie Leboulleux, Martin Schlumberger, _ _
Endocrine-Related Cancer.2018; 25(4): R209. CrossRef - Clinical guidance for radioiodine refractory differentiated thyroid cancer
Matti L. Gild, Duncan J. Topliss, Diana Learoyd, Francis Parnis, Jeanne Tie, Brett Hughes, John P. Walsh, Donald S.A. McLeod, Roderick J. Clifton‐Bligh, Bruce G. Robinson
Clinical Endocrinology.2018; 88(4): 529. CrossRef - Case for Stopping Targeted Therapy When Lung Cancer Progresses on Treatment in Hospice-Eligible Patients
Thomas J. Smith, Nasser Hanna, David Johnson, Sherman Baker, William A. Biermann, Julie Brahmer, Peter M. Ellis, Giuseppe Giaccone, Paul J. Hesketh, Ishmael Jaiyesimi, Natasha B. Leighl, Gregory J. Riely, Joan H. Schiller, Bryan J. Schneider, Joan Tashbar
Journal of Oncology Practice.2017; 13(12): 780. CrossRef - Intermittent Dosing of Dabrafenib and Trametinib in Metastatic BRAFV600E Mutated Papillary Thyroid Cancer: Two Case Reports
Paul S. White, Anita Pudusseri, Stephanie L. Lee, Omar Eton
Thyroid.2017; 27(9): 1201. CrossRef - Aggressive differentiated thyroid cancer with multiple metastases and NRAS and TERT promoter mutations: A case report
Fabiana Pani, Elisabetta Macerola, Fulvio Basolo, Francesco Boi, Mario Scartozzi, Stefano Mariotti
Oncology Letters.2017; 14(2): 2186. CrossRef - Tumors Sharply Increased after Ceasing Pazopanib Therapy for a Patient with Advanced Uterine Leiomyosarcoma: Experience of Tumor Flare
Terumi Tanigawa, Shintaro Morisaki, Hisanobu Fukuda, Shuichiro Yoshimura, Hisayoshi Nakajima, Kohei Kotera
Case Reports in Obstetrics and Gynecology.2017; 2017: 1. CrossRef - Initial Size of Metastatic Lesions Is Best Prognostic Factor in Patients with Metastatic Differentiated Thyroid Carcinoma Confined to the Lung
Mijin Kim, Won Gu Kim, Suyeon Park, Hyemi Kwon, Min Ji Jeon, Jong Jin Lee, Jin-Sook Ryu, Tae Yong Kim, Young Kee Shong, Won Bae Kim
Thyroid.2017; 27(1): 49. CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef - Pharmacodynamic study of axitinib in patients with advanced malignancies assessed with 18F-3′deoxy-3′fluoro-l-thymidine positron emission tomography/computed tomography
Justine Yang Bruce, Peter Colin Scully, Lakeesha L. Carmichael, Jens C. Eickhoff, Scott B. Perlman, Jill Marie Kolesar, Jennifer L. Heideman, Robert Jeraj, Glenn Liu
Cancer Chemotherapy and Pharmacology.2015; 76(1): 187. CrossRef - Optimal Differentiated Thyroid Cancer Management in the Elderly
Donald S. A. McLeod, Kelly Carruthers, Dev A. S. Kevat
Drugs & Aging.2015; 32(4): 283. CrossRef
- Lenvatinib: an investigational agent for the treatment of differentiated thyroid cancer


 KES
KES

 First
First Prev
Prev



